In the world of medical breakthroughs, nature often provides the most unexpected heroes. Imagine harnessing the sting of a honeybee to combat one of humanity’s deadliest foes: breast cancer. In 2020 study revealed that honeybee venom, particularly its star component melittin, can rapidly destroy aggressive breast cancer cells while sparing healthy ones. This discovery, led by Dr. Ciara Duffy at Australia’s Harry Perkins Institute of Medical Research, has sparked excitement for a new era of targeted, natural therapies.
Breast cancer affects millions globally, with over 2.3 million new cases in 2020 alone. Among its subtypes, triple-negative breast cancer (TNBC) and HER2-enriched variants are notoriously aggressive, accounting for 15-20% of cases and resisting standard treatments like hormone therapy. TNBC lacks estrogen, progesterone, and HER2 receptors, making it hard to target, while HER2-enriched tumors overexpress the HER2 protein, fueling rapid growth. Conventional options chemotherapy, radiation, surgery—often bring debilitating side effects, including hair loss, nausea, and immune suppression. The quest for precision medicine has turned eyes to natural compounds, and bee venom emerges as a potent candidate.
The pivotal research, published in npj Precision Oncology, tested venom from over 300 honeybees across Australia, Ireland, and England. Results were striking: at specific concentrations, honeybee venom killed 100% of TNBC and HER2-enriched cells in lab dishes within 60 minutes. Melittin, comprising about 50% of the venom’s dry weight, was the key player. This 26-amino-acid peptide acts like a molecular drill, punching 4-5 nanometer pores into cancer cell membranes. Live-cell imaging showed cells shrinking and lysing rapidly, triggering apoptosis a programmed cell death via caspase activation.
Melittin’s precision stems from its amphipathic structure: one hydrophobic end burrows into lipid bilayers, while a positively charged tail interacts electrostatically with negatively charged cancer membranes. Overexpression of EGFR and HER2 receptors in these cancers amplifies vulnerability. The compound rapidly disrupts oncogenic signaling pathways.
Within 5–20 minutes, it halts phosphorylation of EGFR at Tyr1068 and HER2 at Tyr1248.
As a result, downstream PI3K/Akt and MAPK networks collapse, impairing tumor cell proliferation and survival.
In TNBC models, it even upregulated protective feedback loops in some cells, but overall suppressed growth.
Crucially, melittin spares healthy cells. Tests on normal mammary epithelial cells and fibroblasts showed minimal effects. IC50 values were two to three times higher in non-cancerous cell lines, indicating selectivity. This selectivity helps avoid the collateral damage typical of chemotherapy.
Mutational analyses confirmed the charged C-terminal KRKR sequence as essential for activity.
Neutralizing this region abolished cytotoxic effects.
In contrast, adding targeting motifs such as RGD, which binds integrins, further enhanced tumor specificity.
Why honeybees specifically? Comparisons with bumblebee venom (from Bombus terrestris) highlighted the difference: bumblebee extracts, lacking significant melittin, failed to induce cell death even at high doses. Honeybee venom’s unique composition, including phospholipase A2 and other peptides, synergizes with melittin for enhanced potency. This underscores melittin as the “prominent bioactive anticancer compound” among tested venoms.
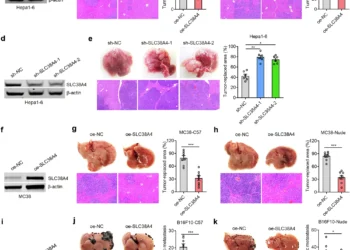
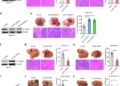
In vivo validation came from mouse models. Injecting melittin into TNBC tumors reduced volume by synergizing with docetaxel, a common chemo agent. Combination therapy slashed proliferation (via Ki-67 markers) to 5.7%, ramped apoptosis to 81%, and downregulated immune evasion protein PD-L1 by 44%. Bioluminescence imaging tracked tumor regression, with effects lasting days.
Advancements have accelerated since 2020. By 2024, researchers paired melittin with the oncolytic coxsackievirus B3 to enhance anti-cancer effects.
In mouse models of breast cancer and melanoma, this combination improved survival by activating immune responses.
In 2025, Dr. Edina Wang’s team engineered melittin with tumor-homing peptides for intravenous delivery.
A single injection triggered tumor cell death within six hours and caused minimal off-target damage in preclinical trials.
Systematic reviews affirm bee venom’s broader anticancer arsenal: inhibiting migration, metastasis, and angiogenesis through gene regulation and cell cycle arrest.
Yet challenges remain. Bee venom can cause allergic reactions, necessitating synthetic or nanoparticle formulations for safe dosing. Human trials are pending, with needs for toxicity studies and optimization across bee genotypes. Cost-effectiveness is a plus venom is abundant worldwide but integrating it with existing therapies like trastuzumab could address resistance.