Dementia affects tens of millions of people worldwide, and projections suggest that number could nearly triple by 2050. Physical activity is a well-established modifiable risk factor. However, most studies have focused on structured exercise rather than movement built into daily life, such as walking to the shops or cycling to meet a friend. To better understand whether cycling linked to lower dementia risk, researchers at Huazhong University of Science and Technology and The University of Sydney examined whether everyday travel mode was associated with dementia risk. They also investigated whether this relationship extended across different dementia subtypes and age groups.

Earlier studies linked active travel to cardiometabolic benefits, including a lower risk of diabetes. Evidence connecting travel habits to brain health, however, remains limited. A 2023 cross-sectional study involving about 32,000 participants in low- and middle-income countries found that low active travel time was associated with higher rates of mild cognitive impairment in adults aged 65 and older. Researchers found no such association in younger adults.
For the current analysis, researchers used data from the UK Biobank. This prospective cohort enrolled more than 500,000 adults aged 40 to 69 in England, Scotland, and Wales between 2006 and 2010. After several exclusions, the final sample included 479,723 participants with a mean age of about 56 years. The team followed them for a median of 13.1 years.
At baseline, participants completed a touchscreen questionnaire and reported the transport modes they used most often during the previous four weeks, excluding work commutes. The researchers classified responses into four groups: nonactive travel, walking only, mixed-walking, and cycling or mixed-cycling. Nonactive travel included cars and public transit. Mixed-walking combined walking with nonactive transport. Cycling or mixed-cycling included cycling alone or cycling with other modes. The team identified dementia cases through linked hospital records and death registries. In a subset of 44,801 participants, researchers also analyzed brain MRI scans.
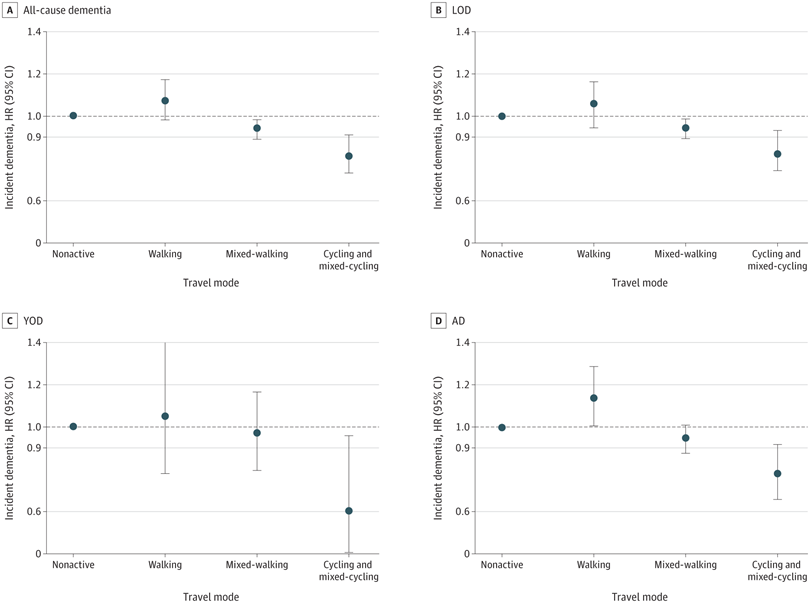
During follow-up, 8,845 participants developed dementia, representing 1.8% of the cohort. The total included 528 cases of young-onset dementia and 3,956 cases of Alzheimer’s disease. Young-onset dementia referred to onset before age 65.
Compared with participants who used nonactive transport, those in the cycling and mixed-cycling group showed a significantly lower hazard of all-cause dementia. The researchers adjusted for age, sex, education, socioeconomic deprivation, body mass index, smoking, alcohol use, overall physical activity, and several chronic diseases. The fully adjusted hazard ratio was 0.81 (95% CI, 0.73–0.91), indicating about a 19% lower observed hazard among cyclists.
This result differs from the widely cited “40% reduction” figure. That estimate applies only to young-onset dementia. In that subgroup, the hazard ratio was 0.60 (95% CI, 0.38–0.95). Because the number of cycling-related cases was small, the confidence interval was wide and the statistical power was limited.
Cycling and mixed-cycling were also associated with lower hazards of late-onset dementia (HR, 0.83) and Alzheimer’s disease (HR, 0.78). Mixed-walking showed a modest reduction in all-cause dementia risk (HR, 0.94). Walking alone did not show the same pattern. Researchers linked it to a slightly higher risk of Alzheimer’s disease (HR, 1.14). The authors said this unexpected finding requires further investigation.
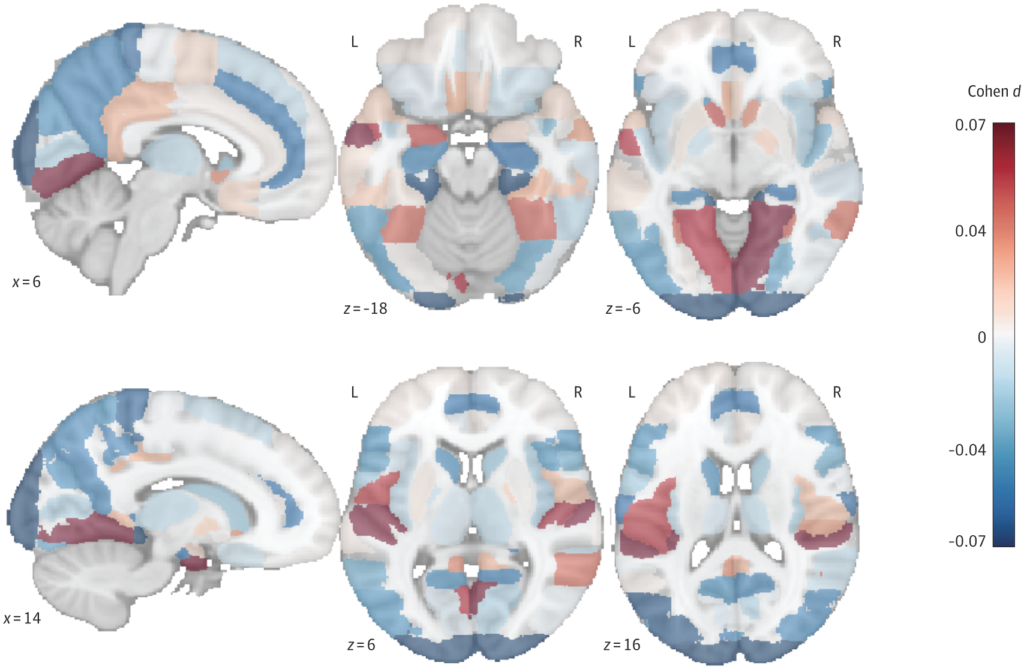
In the neuroimaging subgroup, participants in the cycling and mixed-cycling category had greater gray matter volume in 10 brain regions and larger hippocampal volume. The hippocampus plays a central role in memory and is one of the first structures affected in Alzheimer’s disease. The researchers said these findings provide a possible biological explanation for the observed association.
The study also examined genetic susceptibility. Participants who carried the APOE ε4 allele appeared to derive less benefit from cycling than non-carriers. APOE ε4 is the strongest known genetic risk factor for Alzheimer’s disease. Among non-carriers who cycled, the hazard ratio for all-cause dementia was 0.74. Among ε4 carriers, the hazard ratio was 0.88. This result did not reach statistical significance.
The authors concluded that their findings “suggest an association between active travel mode and incident dementia and brain structure.”
They added that “promoting active travel strategies, particularly cycling, may be associated with lower dementia risk.” Also mentioned that the study was observational and did not establish causation.
Several limitations are important. Participants reported their travel habits only once at baseline, and those habits may have changed during the 13-year follow-up period. Self-reported travel patterns can also introduce measurement error. In addition, more than 94% of the UK Biobank cohort is White, and all participants lived in the United Kingdom. These factors limit how broadly researchers can generalize the findings.
The study cannot determine whether cycling itself reduced dementia risk. People who chose to cycle were generally younger, better educated, and more physically active. They were also less likely to have chronic diseases. The researchers adjusted for these differences, but residual confounding remains possible. Reverse causality is another concern because people in the earliest stages of cognitive decline may stop cycling before receiving a diagnosis. Analyses restricted to employed participants produced similar results. This finding partly addressed the issue, but the authors said they could not eliminate it entirely.
This study identified a strong association between cycling and lower observed dementia risk. It did not prove that cycling prevents dementia. Even so, the findings add to growing evidence that incorporating cycling into everyday travel may support long-term brain health.
Reference:
Hou C, Zhang Y, Zhao F, et al. Active Travel Mode and Incident Dementia and Brain Structure. JAMA Network Open. 2025;8(6):e2514316. doi:10.1001/jamanetworkopen.2025.14316.